
Melasma, often referred to as “the mask of pregnancy,” is a common skin condition that plagues many people, especially pregnant women. Those dark, irregular patches of hyperpigmentation on the face can be a source of both physical and emotional distress. To effectively manage this condition, understanding its causes and available treatment options is essential.
In this comprehensive exploration of melasma, we will take you into the various factors that contribute to its development, discuss whether it is a symptom of underlying issues, and examine the treatments available. While there is no magical overnight cure, patience, diligence, and a tailored approach can lead to meaningful improvements in one’s melasma journey.
What Causes Melasma?
Melasma, often referred to as “the mask of pregnancy,” is a common skin condition characterised by dark, irregular patches of hyperpigmentation on the face. This condition can affect individuals of all skin types and genders, though it is more prevalent in women and those with darker skin tones. While melasma itself isn’t harmful, it can be emotionally distressing for those who experience it. To better understand and manage melasma, it’s essential to explore its causes. In this article, we will delve into the various factors that contribute to the development of melasma.
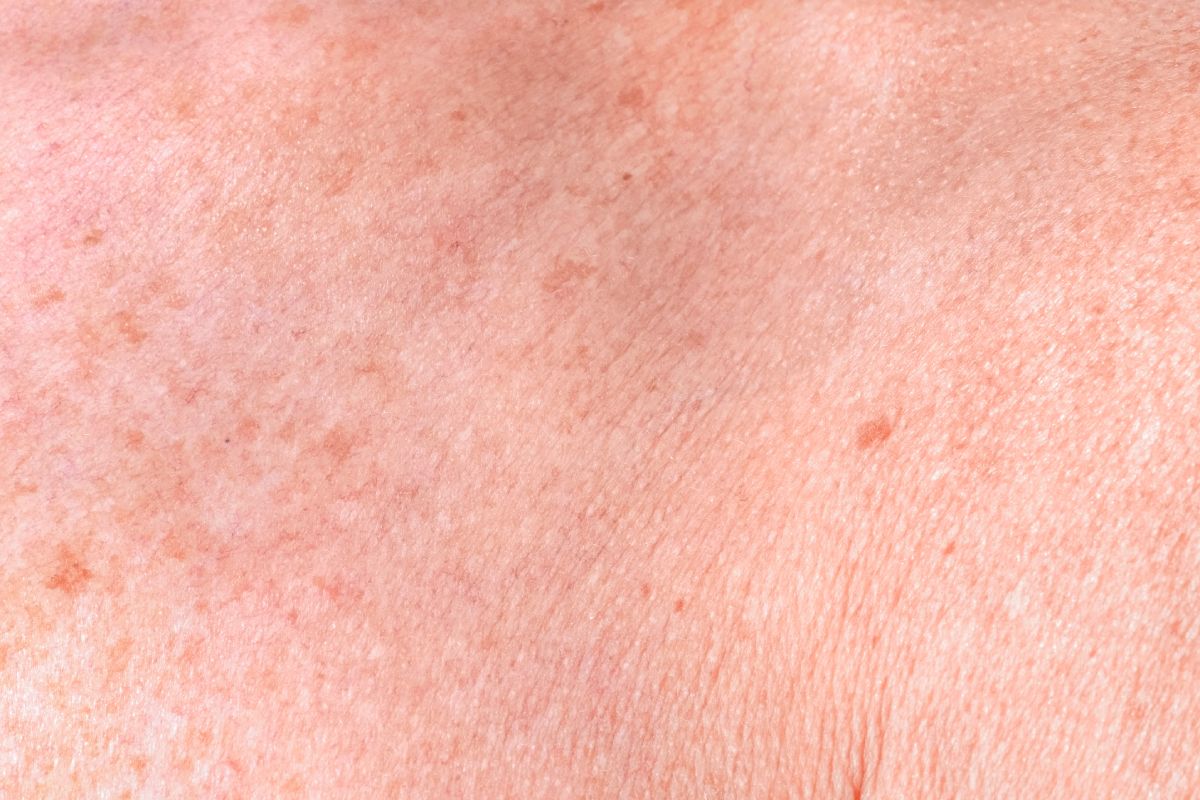
- Hormonal Changes
Hormonal fluctuations are one of the primary causes of melasma. This is why it’s often associated with pregnancy, earning its nickname “the mask of pregnancy.” During pregnancy, the body experiences an increase in the production of hormones like estrogen and progesterone, which can stimulate the melanocytes (pigment-producing cells) in the skin. This increased melanin production results in dark patches on the face.
In addition to pregnancy, hormonal changes related to oral contraceptives and hormone replacement therapy can also trigger melasma in some individuals. Hormonal fluctuations during menopause may contribute to the development of melasma as well.
- Sun Exposure
Sun exposure is a significant external factor that can cause or exacerbate melasma. Ultraviolet (UV) rays from the sun stimulate melanocytes to produce more pigment. Individuals who spend excessive time in the sun without proper sun protection are at a higher risk of developing melasma or making existing melasma worse.
The relationship between sun exposure and melasma is so strong that it’s often said, “Sunscreen is the best treatment for melasma.” Wearing a broad-spectrum sunscreen with a high SPF, along with protective clothing and accessories like wide-brimmed hats, is essential for preventing and managing melasma.
- Genetic Predisposition
Genetics also play a role in the development of melasma. If you have a family history of melasma, you may be more susceptible to it. Specific genetic factors may influence how your skin responds to hormonal changes and sun exposure, making you more prone to developing melasma under certain conditions.
- Skin Type and Ethnicity
Melasma is more commonly observed in individuals with darker skin tones, including those of Hispanic, Asian, African, and Middle Eastern descent. People with Fitzpatrick skin types III to VI are more susceptible to melasma. This is because their skin contains more melanin, which provides some natural protection against the harmful effects of UV rays but can also lead to increased pigmentation when stimulated by hormonal changes.
- Other Triggers
Apart from hormonal changes, sun exposure, genetics, and skin type, other factors can contribute to the development of melasma. These may include:
- Medications: Certain medications, such as antiseizure drugs, may increase the risk of melasma as a side effect.
- Cosmetics and skin care products: The use of certain cosmetics or skincare products that irritate the skin or cause inflammation can exacerbate melasma.
- Heat: Prolonged exposure to heat, such as from hot baths or saunas, may worsen melasma.

Is Melasma a Symptom of Something Else?
Melasma, characterised by the development of dark, irregular patches on the face, can be a distressing skin condition on its own. However, it’s essential to consider whether melasma could be a symptom of an underlying medical issue or a side effect of other conditions. In this section, we will explore whether melasma is typically a standalone concern or if it can be an indicator of something else.
- Hormonal Imbalances
As mentioned in the previous section, hormonal changes are a primary cause of melasma. While melasma itself is not usually a symptom of hormonal imbalances, the conditions that cause hormonal imbalances can sometimes lead to melasma as a secondary effect.
For example, polycystic ovary syndrome (PCOS), a hormonal disorder in women, can result in elevated levels of androgens (male hormones) and insulin resistance. These hormonal imbalances can indirectly trigger melasma by influencing melanin production. So, while melasma is not a direct symptom of PCOS, it can occur more frequently in individuals with this condition.
- Adrenal Gland Disorders
Some adrenal gland disorders, such as Addison’s disease and Cushing’s syndrome, can cause hormonal imbalances. Cushing’s syndrome, in particular, is associated with elevated cortisol levels, which can affect the skin and may potentially contribute to melasma.
- Medications
Certain medications, including antiseizure drugs, contraceptive pills, and hormone replacement therapy, can increase the risk of melasma as a side effect. However, this does not necessarily mean that melasma is a symptom of the underlying condition being treated with these medications. Instead, it’s a known side effect of the drugs themselves.
- Thyroid Disorders
Thyroid disorders, such as hypothyroidism and hyperthyroidism, can affect the body’s hormonal balance. While thyroid disorders don’t directly cause melasma, they can lead to skin changes, including dryness, which may exacerbate melasma and other skin issue such as acne.
- Other Dermatological Conditions
Melasma is primarily a skin condition, but it can sometimes coexist with or be mistaken for other dermatological issues. For instance, post-inflammatory hyperpigmentation (PIH) is another skin condition that can resemble melasma but is caused by skin trauma or inflammation rather than hormonal factors.
- Psychological and Emotional Factors
While not a direct symptom of psychological or emotional conditions, melasma can have a significant impact on an individual’s self-esteem and emotional well-being. The visible nature of melasma can lead to feelings of self-consciousness, anxiety, or depression, highlighting the importance of addressing the emotional aspects of dealing with melasma.
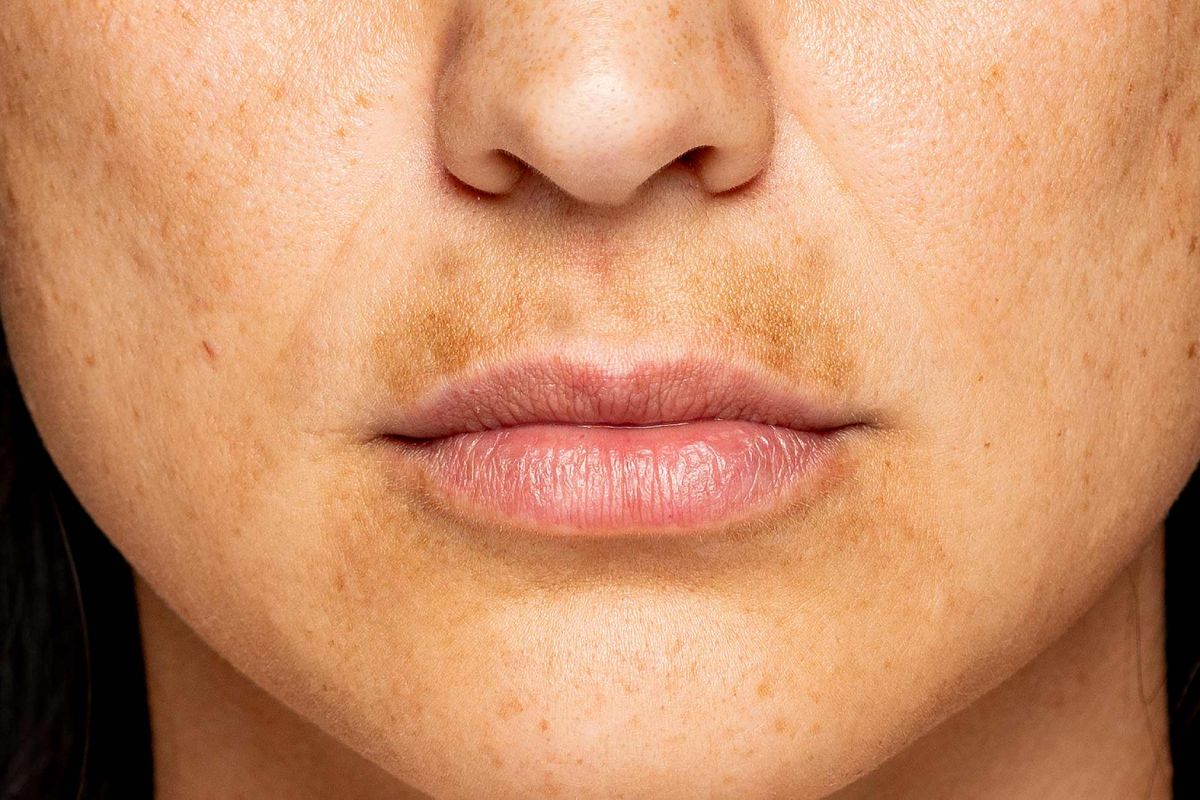
What’s the Fastest Way to Treat Melasma?
Melasma can be a challenging skin condition to treat, and there is no “fast cure” that can eliminate it overnight. Effective treatment requires patience, consistent effort, and a combination of various approaches. In this section, we will explore the available treatment options for melasma, emphasising that while there is no instant solution, some methods can produce noticeable improvements over time.
- Sun Protection: Sun exposure is a major exacerbating factor for melasma. Therefore, the first and foremost step in managing melasma is diligent sun protection. This includes wearing broad-spectrum sunscreen with a high SPF daily, even on cloudy days. Additionally, wearing protective clothing such as wide-brimmed hats and sunglasses can help shield the skin from harmful UV rays.
- Topical Treatments: Several topical treatments can help fade melasma over time. These often include:
- Hydroquinone: A skin-lightening agent available in both prescription and over-the-counter forms. It works by reducing the production of melanin.
- Retinoids: Topical retinoids like tretinoin can help improve the appearance of melasma by promoting skin cell turnover.
- Topical Steroids: In some cases, topical steroids may be prescribed to reduce inflammation and pigmentation.
- Combination Creams: Some products combine hydroquinone, retinoids, and a steroid to target melasma from multiple angles.
- Chemical Peels: Chemical peels, administered by a dermatologist, can help remove the top layer of skin, where melasma pigmentation resides. This can lead to a more even skin tone over time.
- Microneedling: Microneedling involves using tiny needles to create micro-injuries in the skin, stimulating collagen production and potentially improving the appearance of melasma. It is often combined with topical treatments.
- Laser Therapy: Laser treatments, such as fractional laser and intense pulsed light (IPL), can target melanin and break it down. These treatments can be effective, but they may require multiple sessions and downtime.
- Cosmetic Camouflage: Makeup can provide a quick and temporary solution to cover melasma. Look for makeup products designed to conceal hyperpigmentation.
- Oral Medications: In some cases, oral medications like tranexamic acid may be prescribed to help manage melasma. These are typically used when other treatments have not produced satisfactory results.
It’s essential to note that the effectiveness of these treatments can vary from person to person. What works best for one individual may not be as effective for another. Additionally, melasma has a tendency to recur, especially if sun protection measures are not maintained.
The fastest way to achieve visible improvement in melasma is often a combination of treatments under the guidance of a dermatologist. However, even with a comprehensive treatment plan, it may take several weeks or months to see significant results.
Conclusion
Melasma, with its intricate web of causes and complexities, demands a multifaceted approach for effective management. Understanding the factors that contribute to melasma’s development is the first step in the journey.
While melasma itself is not typically a symptom of underlying medical issues, it can sometimes be associated with conditions like PCOS and adrenal gland disorders.
However, addressing melasma primarily involves a combination of diligent sun protection, topical treatments, and advanced therapies under the guidance of a dermatologist. The path to clearer skin may not be the fastest, but with patience and a tailored approach, it is indeed achievable.
Remember, consulting with healthcare professionals for personalised advice and treatment options is key to successfully managing and living with melasma.

